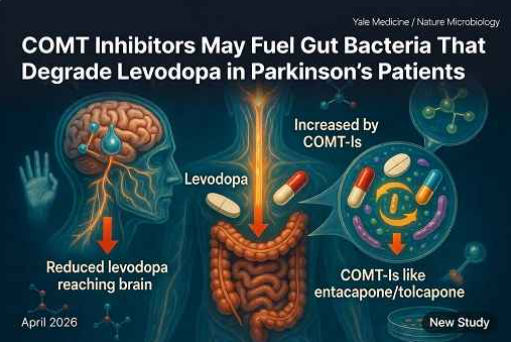
Washington: A new study has revealed a previously unknown interaction between two cornerstone Parkinson’s disease medications that could unintentionally reduce treatment effectiveness in some patients. Researchers at Yale School of Medicine found that catechol-O-methyltransferase inhibitors (COMT-Is)—drugs commonly prescribed alongside levodopa to prolong its action—can reshape the gut microbiome in ways that promote the growth of bacteria capable of breaking down levodopa before it reaches the brain.
Parkinson’s disease is a progressive neurodegenerative disorder characterized by the loss of dopamine-producing neurons in the brain, leading to motor symptoms such as tremors, rigidity, and bradykinesia. Levodopa remains the gold-standard therapy because it crosses the blood-brain barrier and is converted into dopamine. However, much of the oral dose is metabolized peripherally before reaching the central nervous system. To counter this, physicians often add COMT inhibitors (such as entacapone, tolcapone, or opicapone) and aromatic L-amino acid decarboxylase (AADC) inhibitors like carbidopa. These adjuncts were designed to extend levodopa’s half-life and improve symptom control.
The Yale team, led by postdoctoral associate Andrew A. Verdegaal, PhD, and senior author Andrew Goodman, PhD, discovered an unexpected downside. Using ex-vivo experiments with human fecal microbial communities from multiple donors, the researchers demonstrated that COMT-Is possess antibacterial properties. These drugs selectively kill off certain susceptible gut bacteria, allowing more resilient species—particularly Enterococcus faecalis—to proliferate. E. faecalis carries the tyrosine decarboxylase (tyrDC) gene, whose enzyme converts levodopa into dopamine directly in the gut. Because dopamine cannot cross the blood-brain barrier, this microbial metabolism reduces the amount of levodopa available for therapeutic benefit.
The study, published April 6, 2026, in Nature Microbiology, showed clear, individual-specific shifts in microbiome composition and levodopa metabolism after COMT-I exposure. In some fecal communities, treatment with tolcapone (a COMT-I) significantly increased Enterococcus abundance and accelerated the breakdown of deuterated levodopa (L-DOPA-d3) into dopamine and downstream metabolites. When researchers added wild-type E. faecalis to a community lacking detectable Enterococcus, levodopa degradation rose sharply in the presence of the inhibitor—confirming the drug–microbiome–drug interaction.
Lead author Verdegaal summarized the counterintuitive finding: “We found a counterproductive effect of this drug that’s meant to increase levodopa efficacy… While we generally think of the liver as the mediator for drug-drug interactions, this interaction occurs instead through the gut microbiome.”
The discovery builds on earlier research showing that certain gut bacteria (including Enterococcus and Eggerthella species) can metabolize levodopa, contributing to variable patient responses and “off” periods. However, this is the first demonstration that a co-prescribed Parkinson’s medication can actively drive the enrichment of these levodopa-metabolizing microbes.
Implications for Patients and Future Care
The findings suggest that microbiome composition may help explain why some patients respond better than others to standard levodopa-plus-COMT-I regimens. Personalized approaches—such as microbiome profiling before starting therapy, targeted antibiotics, or probiotic interventions—could one day optimize treatment. The study also highlights the broader importance of considering the gut microbiome in drug development and polypharmacy decisions for chronic neurological conditions.
References:
Verdegaal, A.A. et al. (2026). “A drug–microbiome–drug interaction impacts co-prescribed medications for Parkinson’s disease.” Nature Microbiology. https://www.nature.com/articles/s41564-026-02299-2
Yale School of Medicine News. (2026). “New Study Finds Counterproductive Effect of Parkinson’s Disease Drug.” https://medicine.yale.edu/news-article/counterproductive-effect-of-parkinsons-disease-drug/
MedicalXpress. (2026). “Parkinson’s add-on drugs may spur gut bacteria that break down levodopa, study finds.” https://medicalxpress.com/news/2026-04-parkinson-drugs-spur-gut-bacteria.html
Acknowledgement: This news draft draws directly from the primary research conducted by the Goodman Lab at Yale School of Medicine and the peer-reviewed publication in Nature Microbiology. Special thanks to the study authors for making their findings publicly accessible through institutional press releases and open summaries, enabling timely public understanding of this important microbiome–drug interaction.





